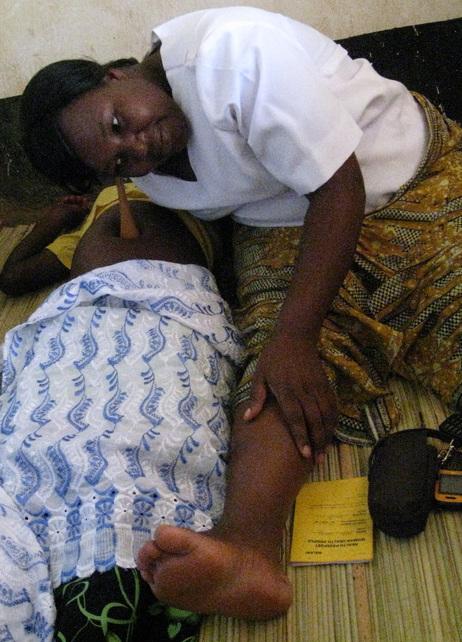
Chipondwe Ante-natal visit
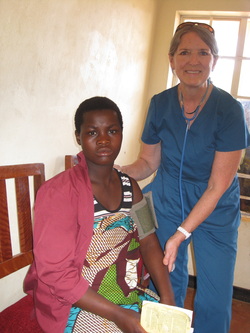
Dec. 20, Ante-natal monitoring in Chipondwe
St. Gabriel's Hospital has a Mobile Health Unit that visits 21 villages in their catchment area and offers a variety of immunization, ante-natal clinics, HIV testing, as well as monitoring of children for malnutrition. I asked Matron Hilda if I could accompany the team on a visit and was referred to the Tuesday Ante-natal clinic in Chipondwe, a village about 30 minutes west of Namitete. Maternal and Child Health is a particular interest of mine and I looked forward to assessing how the health care needs of this specific group were addressed.
Tuesday morning dawned hot and bright and I awakened early. The downpours have stopped, and irrigation systems have begun operating in the local fields. World wide weather systems vary everywhere and I was reminded that even in the "rainy season" in Malawi, the weather has become unpredictable.
I packed up my backpack and met with the Mobile Health Team at 0730 at the Outpatient building. The team consists of one nurse/midwife (Hellen), a ward assistant (Mariana), a Health Surveillance Assistant (Gift), who is Manager of Community Health Needs, collator of records and HIV Counselling and Testing technician; and a driver.
I was really pleased to see that our Toyota truck was donated by World Vision International! I later heard from the technician, that World Vision is doing an amazing job in Chipondwe, assisting farmers with increasing crop yield, housing, and educational support.
Mariana and I climbed into the back of the truck, along with HIV Rapid Test equipment, health records, a weigh scale, vitamin supplements and a bamboo mat. We sat on foam pads which made the trip fairly comfortable.
Our highway drive took us past large tracts of tobacco fields (Malawi's biggest export), cassava bushes, low plantings of ground nuts, and easily recognized maize; everything appearing bright green and lush against the reddish soil.
Our first stop came at a police check between Lilongwe and Namitete district boundaries. Police checks have recently become more frequent on the highways, ostensibly to check on seat belt usage (as if! there are at least twice the number of people in a vehicle as there are seat belts!). The government is more likely monitoring the activities of protesting youth militia. In any case, we sat as a policeman approached from a roadside hut and gave the vehicle a once over. He peered into the back, spied the weigh scale, reached in and removed it! Before I could warrant a guess as to what was going on, he stepped onto the scale and cheerily called out to a colleague, "70 kgs!" The weigh scale was then returned, and we were waved on our way.
A Malawi moment.
After a short off-road route we arrived in a central area of Chipondwe, a thatch roofed rural site. A large number of pregnant women were already congregating in front of a 4 room brick house where the clinic would be held.
I am aware that these women are particularly fortunate. Because they fall into the St. Gabriel's catchment area, they receive best available ante-natal monitoring and obstetrical care. This is not the case in many parts of Malawi.
A little background:
Culturally, Malawians value large families, and women in Malawi on average, give birth five times in their lifetime. Women do not have equality in marital relationships and cannot refuse sex. Birth control options are limited to non-existent. The continued increase in population is an on-going concern for a country struggling with development needs. Traditionally, women have given birth in their homes with the assistance of female relatives or T.B.A.'s (traditional birth attendants). Most of these traditional midwives have no medical training. It is extremely common for unmonitored women to experience complications during birth; complications which can lead to the death of mother, baby, or both. According to the World Health Organization, post-partum haemorrhage is the leading cause of maternal mortality. Birth asphyxia and neonatal sepsis are leading causes of infant mortality.
To address these issues, the Malawian government passed a law in 2007, requiring all women to give birth at a local health care facility. Village chiefs threatened families that a goat would be taken from them if a woman delivered at home. However, the law was rescinded in 2010, due to the overwhelming number of pregnant women presenting at poorly staffed labour wards. The government now offers training to T.B.A.'s, but this is a hit and miss solution. The Malawi Ministry of Health (2011) confirms that giving birth in Malawi still carries a lifetime risk of maternal death, at 1:7.
Back to Chipondwe:
The team sets up an assessment room for weights and blood pressures, and an HIV assessment room. The women, clothed in colourful chitenje cloths, file in, one by one. Another group of women are seated outside under shade trees and are selling fried maize buns and drinks. It appears that this will be an all-day affair!
A typical ante-natal screening clinic sees at least 100 women. All new patients must purchase an ante-natal health passport and take an HIV rapid test. I see several patients with elevated B.P.'s and swollen ankles and Hellen instructs them to travel to St. Gabriel's for a clinical consult. I recognize one of the women 2 days later at the hospital, so know they take the advice they've received, seriously. Women tested as HIV positive are referred to the ART Clinic for education and treatment. Their husbands are also asked to come in for testing.
After vital signs and HIV testing, Hellen begins fetal assessment. She spreads out the bamboo mat in a small 9X9 foot room, seats herself in the middle and calls for the first 2 women to enter. They lie on either side of her, raise their tops and she expertly uses her hands to assess size and position of the fetus. She speaks briefly with each one. Then, with a small wooden fetalscope, she listens for heartbeats, writes in their passports and readies herself for the next two women. It's an ingenious arrangement that allows Hellen to see a large number of clients in a shorter length of time.
Women make a final visit to the ward assistant, who makes an entry into their health passport and hands out small paper wrapped packages of vitamins, plus a combination of magnesium, iron, zinc and calcium.
It has been a long, hot day without breaks, in a dusty, barren group of village houses. It has also been an impressive day.
Women we have seen have been well monitored to ensure they have healthy pregnancies and deliver healthy babies.
There were 2,979 deliveries last year, 52 neonatal deaths - a 21% decrease since 2009.
Even though health care resources in Malawi are stretched to the limit, good things are happening in this catchment area.
Photos below:
Tuesday morning dawned hot and bright and I awakened early. The downpours have stopped, and irrigation systems have begun operating in the local fields. World wide weather systems vary everywhere and I was reminded that even in the "rainy season" in Malawi, the weather has become unpredictable.
I packed up my backpack and met with the Mobile Health Team at 0730 at the Outpatient building. The team consists of one nurse/midwife (Hellen), a ward assistant (Mariana), a Health Surveillance Assistant (Gift), who is Manager of Community Health Needs, collator of records and HIV Counselling and Testing technician; and a driver.
I was really pleased to see that our Toyota truck was donated by World Vision International! I later heard from the technician, that World Vision is doing an amazing job in Chipondwe, assisting farmers with increasing crop yield, housing, and educational support.
Mariana and I climbed into the back of the truck, along with HIV Rapid Test equipment, health records, a weigh scale, vitamin supplements and a bamboo mat. We sat on foam pads which made the trip fairly comfortable.
Our highway drive took us past large tracts of tobacco fields (Malawi's biggest export), cassava bushes, low plantings of ground nuts, and easily recognized maize; everything appearing bright green and lush against the reddish soil.
Our first stop came at a police check between Lilongwe and Namitete district boundaries. Police checks have recently become more frequent on the highways, ostensibly to check on seat belt usage (as if! there are at least twice the number of people in a vehicle as there are seat belts!). The government is more likely monitoring the activities of protesting youth militia. In any case, we sat as a policeman approached from a roadside hut and gave the vehicle a once over. He peered into the back, spied the weigh scale, reached in and removed it! Before I could warrant a guess as to what was going on, he stepped onto the scale and cheerily called out to a colleague, "70 kgs!" The weigh scale was then returned, and we were waved on our way.
A Malawi moment.
After a short off-road route we arrived in a central area of Chipondwe, a thatch roofed rural site. A large number of pregnant women were already congregating in front of a 4 room brick house where the clinic would be held.
I am aware that these women are particularly fortunate. Because they fall into the St. Gabriel's catchment area, they receive best available ante-natal monitoring and obstetrical care. This is not the case in many parts of Malawi.
A little background:
Culturally, Malawians value large families, and women in Malawi on average, give birth five times in their lifetime. Women do not have equality in marital relationships and cannot refuse sex. Birth control options are limited to non-existent. The continued increase in population is an on-going concern for a country struggling with development needs. Traditionally, women have given birth in their homes with the assistance of female relatives or T.B.A.'s (traditional birth attendants). Most of these traditional midwives have no medical training. It is extremely common for unmonitored women to experience complications during birth; complications which can lead to the death of mother, baby, or both. According to the World Health Organization, post-partum haemorrhage is the leading cause of maternal mortality. Birth asphyxia and neonatal sepsis are leading causes of infant mortality.
To address these issues, the Malawian government passed a law in 2007, requiring all women to give birth at a local health care facility. Village chiefs threatened families that a goat would be taken from them if a woman delivered at home. However, the law was rescinded in 2010, due to the overwhelming number of pregnant women presenting at poorly staffed labour wards. The government now offers training to T.B.A.'s, but this is a hit and miss solution. The Malawi Ministry of Health (2011) confirms that giving birth in Malawi still carries a lifetime risk of maternal death, at 1:7.
Back to Chipondwe:
The team sets up an assessment room for weights and blood pressures, and an HIV assessment room. The women, clothed in colourful chitenje cloths, file in, one by one. Another group of women are seated outside under shade trees and are selling fried maize buns and drinks. It appears that this will be an all-day affair!
A typical ante-natal screening clinic sees at least 100 women. All new patients must purchase an ante-natal health passport and take an HIV rapid test. I see several patients with elevated B.P.'s and swollen ankles and Hellen instructs them to travel to St. Gabriel's for a clinical consult. I recognize one of the women 2 days later at the hospital, so know they take the advice they've received, seriously. Women tested as HIV positive are referred to the ART Clinic for education and treatment. Their husbands are also asked to come in for testing.
After vital signs and HIV testing, Hellen begins fetal assessment. She spreads out the bamboo mat in a small 9X9 foot room, seats herself in the middle and calls for the first 2 women to enter. They lie on either side of her, raise their tops and she expertly uses her hands to assess size and position of the fetus. She speaks briefly with each one. Then, with a small wooden fetalscope, she listens for heartbeats, writes in their passports and readies herself for the next two women. It's an ingenious arrangement that allows Hellen to see a large number of clients in a shorter length of time.
Women make a final visit to the ward assistant, who makes an entry into their health passport and hands out small paper wrapped packages of vitamins, plus a combination of magnesium, iron, zinc and calcium.
It has been a long, hot day without breaks, in a dusty, barren group of village houses. It has also been an impressive day.
Women we have seen have been well monitored to ensure they have healthy pregnancies and deliver healthy babies.
There were 2,979 deliveries last year, 52 neonatal deaths - a 21% decrease since 2009.
Even though health care resources in Malawi are stretched to the limit, good things are happening in this catchment area.
Photos below: